Most transparency reforms aim to correct perceived misaligned incentives in the biopharmaceutical marketplace. However, many efforts to mandate information flow in the private market have serious consequences for every stakeholder in the market, including patients.
One proposal gaining popularity nationwide is advance price notification. This new rule would require biopharmaceutical manufacturers to submit reports to public and private insurers, including pharmacy benefit managers (PBMs), relaying increases in the list price of a medicine prior to the increase taking effect in the market. The proponents of these proposals insist that patients and payers deserve pricing transparency, but they fail to recognize the real hurdles and risks caused by advance price notification.
Advance notification of price increases does not save money for patients or payers, including the government.
For patients: Out-of-pocket costs for a medicine are determined by a patient’s insurer and PBM. Mandatory price reporting of a medicine’s list price has little impact on what patients actually pay because it does not reflect the rebates or discounts their insurer or PBM receive for the medicine, which impacts the level of insurance coverage for that medicine and determines the patient’s final take-home cost.
For payers: State and federal agencies that purchase prescription drugs would be tasked with managing the complexities and additional administrative burdens of constant price revisions.
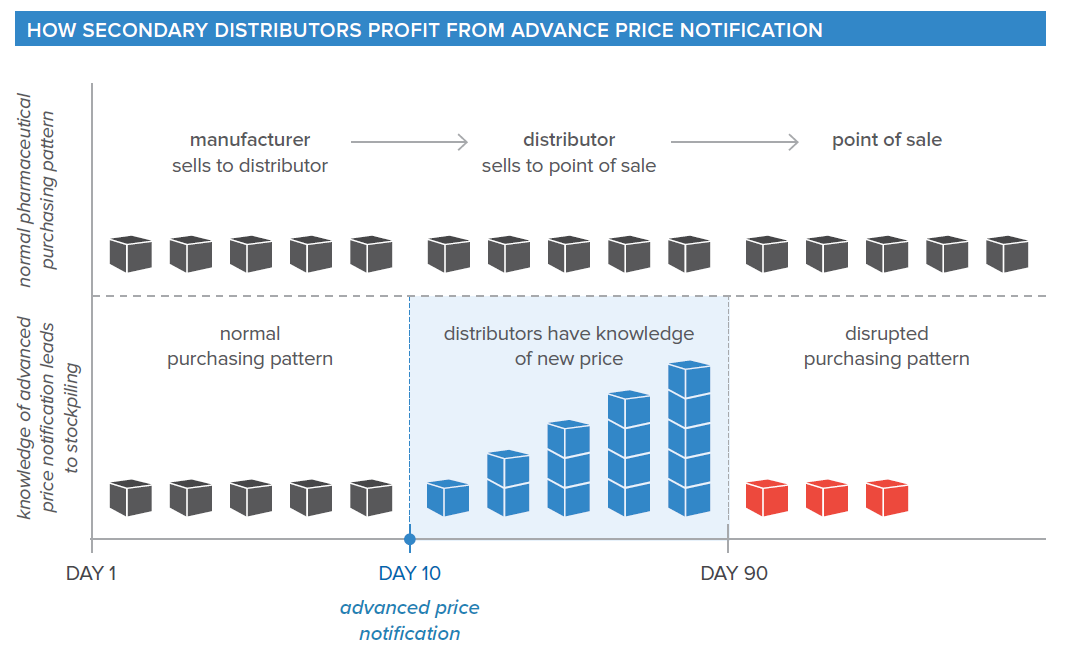
Advance notification of price increases could lead to speculative purchasing, or distorted market power, in the prescription drug supply chain.
Advance price notification measures would threaten years of work by regulators and industry to eradicate practices to profit from fluctuations in price. By notifying payers of anticipated price increases in advance, distributors – especially those that do not previously negotiate contractual agreements with manufacturers – are incentivized to purchase and stockpile medicines at the old price, and wait to sell them at the new price once the increase goes into effect. In the past, this has resulted in prices going up, not down, for the entire supply chain.
Advance notification of price increases could cause medicine shortages for patients.
Medicine shortages are caused by a wide variety of market complications, such as lack of raw materials from suppliers or discontinuations of medicine. They can also be caused by disturbances within the pharmaceutical supply chain. If distributors are incentivized to hoard medicine after learning of an upcoming price increase from a required advance price notification, they could cause a shortage in the market of that medicine by purchasing large quantities of it at the lower price. Such behavior has occurred in the past where providers and patients were not able to access the medicines they needed because the distribution channel was gummed up by such misaligned incentives. These market distortions have largely been eliminated, but could return because of advance price notification provisions.
Regulators and industry leaders have worked for decades to ensure the biopharmaceutical supply chain remains a robust marketplace for payers and patients. Proposals to reveal business critical, proprietary information in advance of formal release will jeopardize the market-based mechanisms that deliver new and affordable medicines to patients.
To learn more about the actual impact of advance price notifications, see here.




