Earlier this year, PhRMA released a proactive agenda with common-sense, patient-centered reforms to improve access to quality, affordable health care. The urgency of building a stronger, more resilient health care system is apparent in light of new data from the U.S. Centers for Disease Control and Prevention that show an increasing number of deaths from heart disease, diabetes and other chronic conditions in the wake of the COVID-19 pandemic. Alarmingly, in 2020, Americans experienced the largest drop in average life expectancy since World War II.
Improving medication utilization and adherence can help to curb this alarming trend and improve health outcomes. Take patients with diabetes. Research clearly shows that lower medication adherence is associated with avoidable health complications, higher costs for the health care system, more missed days of work and school, and decreased quality of life. Here are three key factors impacting medicine adherence for diabetes patients:
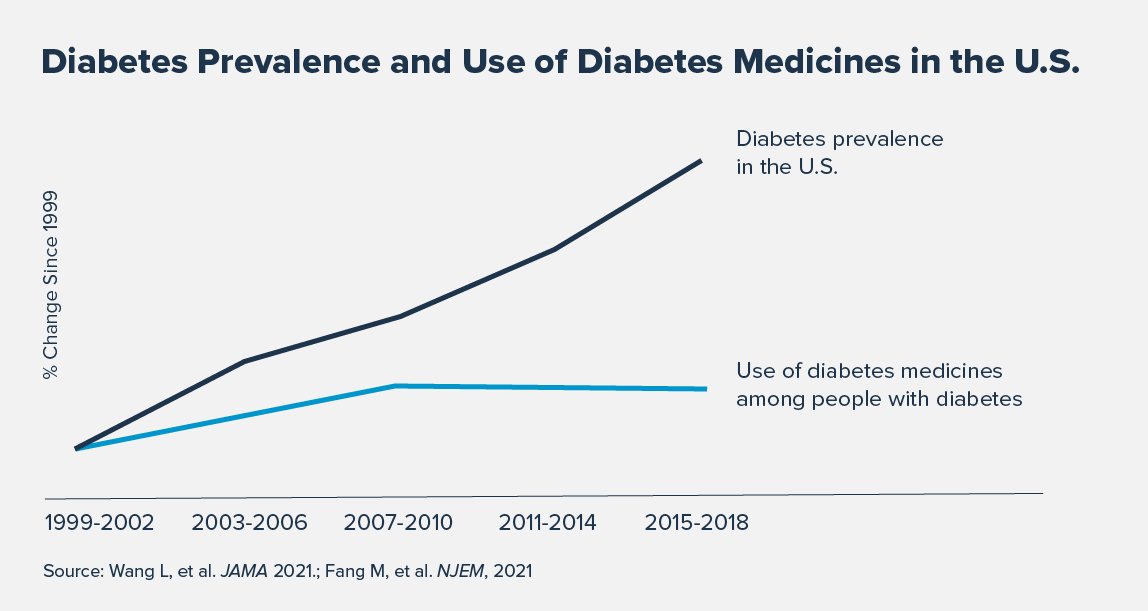
1. Undertreatment. Recent studies in the Journal of the American Medical Association (JAMA) and The New England Journal of Medicine (NEJM) show a concerning decline in the share of people with diabetes who have well-controlled blood sugar, blood pressure, and cholesterol levels. The data also show that the use of diabetes medicines has failed to keep pace with the growing prevalence of the condition. Undertreatment and poor adherence among patients with diabetes raises the risk of complications, such as cardiovascular events and microvascular disease (which can lead to kidney failure, blindness or amputation), and likely contributed to the 14% increase in diabetes-related deaths in 2020.
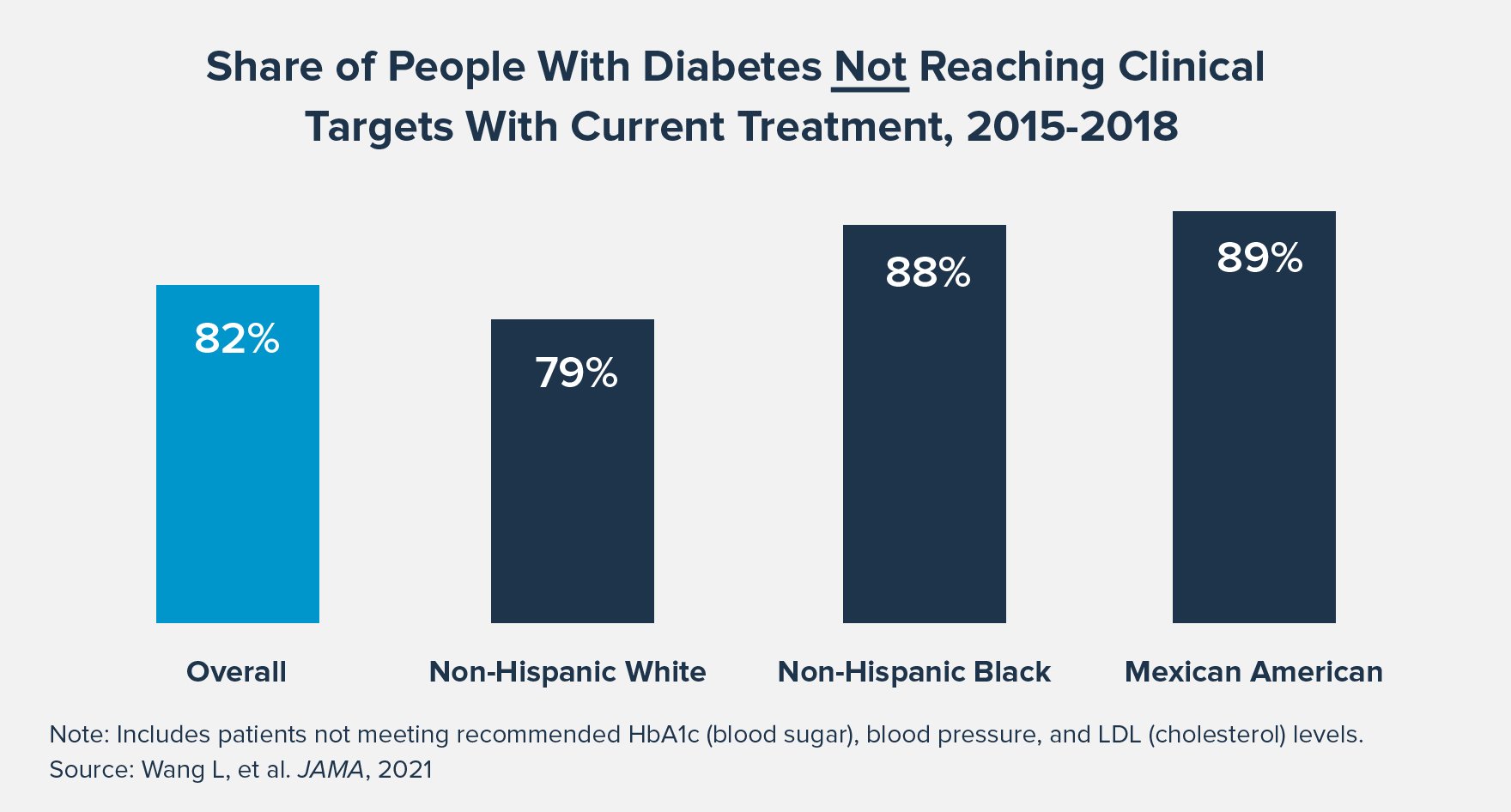
2. Health disparities. Fewer than 1 in 5 U.S. adults with diabetes are meeting recommended clinical goals with their existing treatment regimens. Among patients with poorly controlled diabetes, Mexican and Black Americans are less likely to receive adequate treatment compared to non-Hispanic white Americans. This disparity in medicine use and disease management may help to explain why racially/ethnically diverse communities are disproportionately more likely to experience diabetes-related complications and death.
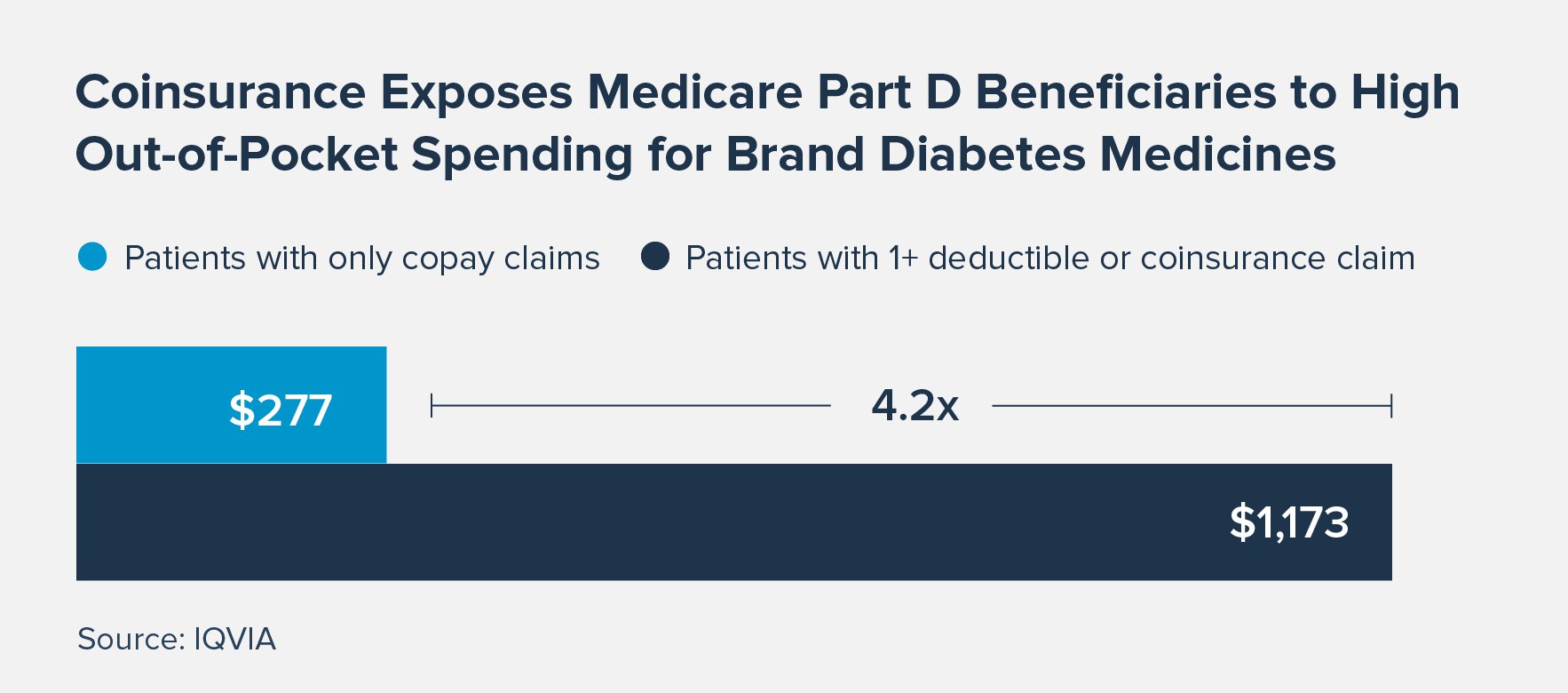
3. High out-of-pocket costs. Over the past two decades, many Medicare beneficiaries with deductibles and coinsurance have faced growing out-of-pocket costs for their diabetes medicines. Beneficiaries with coinsurance and deductibles taking brand diabetes medicines spend, on average, more than four times more out of pocket compared to beneficiaries with only copays. These high costs can create a significant barrier to patient adherence.
Reducing financial barriers can help improve patient adherence to medicine. One recent study found that eliminating cost sharing for medicines to treat certain chronic conditions, including diabetes, significantly increased patient adherence and resulted in an average of $63 (10%) savings per member per month, even after accounting for the cost of medicines.
Our proactive agenda includes reforms that would lower medicine costs and help improve adherence for patients by:
- Modernizing how Medicare covers and pays for medicines, including capping out-of-pocket costs in Part D, lowering cost sharing, and spreading patient costs over the calendar year;
- Making insurance work like insurance by covering more medicines from day one, making out-of-pocket costs more predictable, and sharing negotiated savings with patients at the pharmacy counter; and
- Building a more just, equitable health care system by improving data collection and reporting that more accurately measures health disparities and promoting best practices for improving equity in health care screenings, diagnosis and treatment.
America's biopharmaceutical research industry is ready to do its part to help ensure all patients can afford and access the medicines they need. To learn more, visit www.phrma.org/BetterWay.






