Patients, especially those suffering from chronic conditions, deserve access to the medicines they need to live longer, healthier lives. Today, PhRMA released a new fact sheet on access to asthma medicines in exchange plans in 2015 (2014 fact sheet is available here). The fact sheet highlights some of the potential barriers to accessing needed treatments. Learn more on AccessBetterCoverage.org, in our patient profiles and our other fact sheets.
This is the fourth post in our Burden on Patients Q&A series with patient advocates. To learn more, we asked Meryl Bloomrosen, senior vice president, policy, advocacy and research at the Asthma and Allergy Foundation of America, to answer a few questions.
Question: What is the Asthma and Allergy Foundation of America (AAFA) (www.aafa.org) and who do you represent?

Answer: AAFA is a not-for-profit patient organization whose mission is to improve the quality of life for over 60 million Americans who suffer from asthma and allergic diseases. More people than ever are struggling to live normal and healthy lives in the face of the daily limits that asthma and other allergic diseases create. Our goal is to help them to manage their lives and their health, through education, advocacy, and research. We develop and disseminate information and educational resources. We also work to educate and raise awareness about asthma and allergies, to promote access to affordable, quality healthcare, and to promote prevention, screening and lifestyle interventions that reduce the incidence and adverse effects of asthma and allergies.
Q: How do medicines help patients manage and treat asthma?
A: Medicines are critical to helping patients with asthma manage their health. In general, medicines are directed either toward control (preventing and reducing inflammation that causes airway narrowing that puts the patient at risk for an acute asthma episode) or rescue (reducing airway constriction, in a patient who is experiencing symptoms/who has an asthma attack). Medications are one very important aspect of treatment. But it is also very important that people with asthma pay attention to their environment. People need be able to reduce exposure to the triggers (such as allergens, dust, and airborne chemicals) that cause acute episodes. That requires attention to the home, and school, and workplace; and education about what are the asthma triggers and how exposure to them can be minimized.
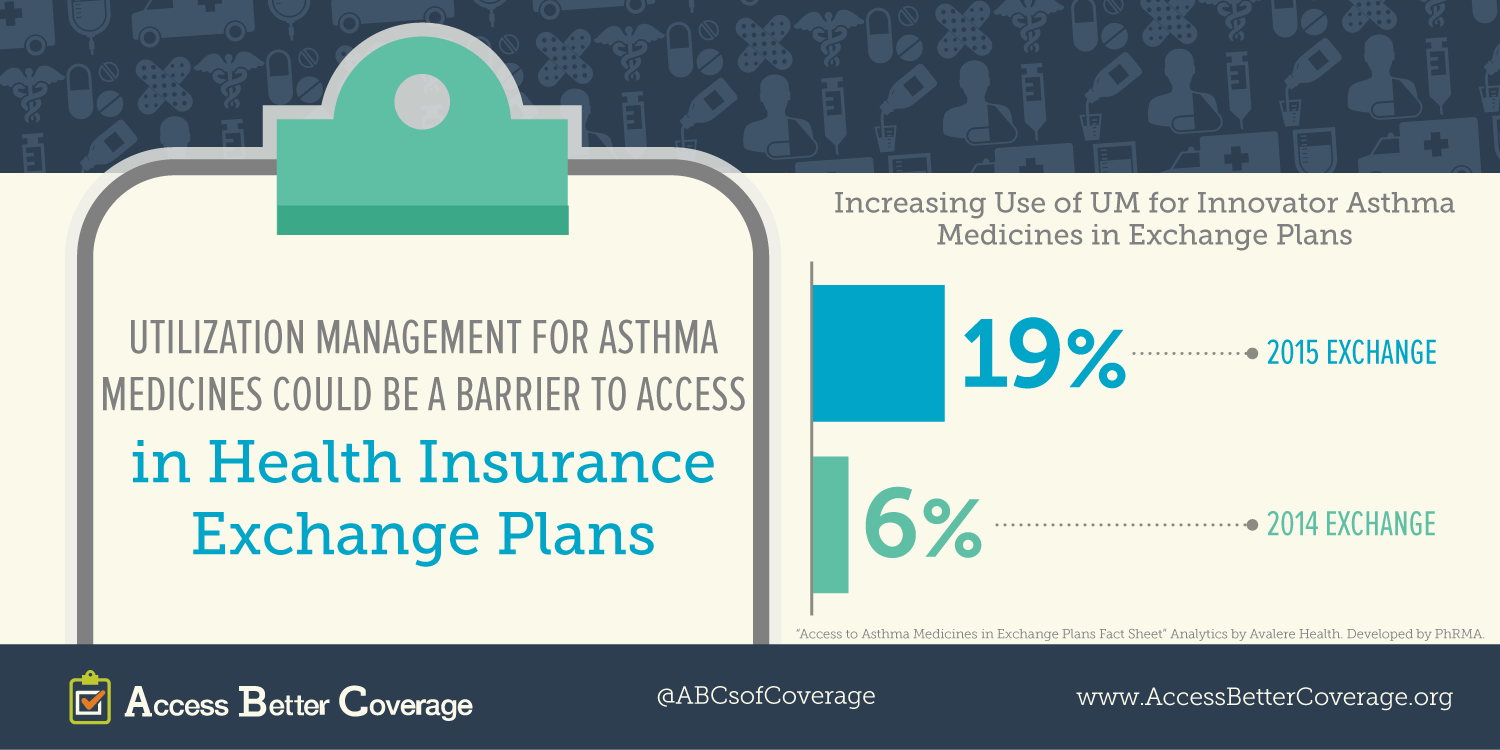 Q: The Affordable Care Act (ACA) expanded health insurance coverage to a broader population. What are you hearing about coverage in health insurance exchanges, in particular access to asthma medicines?
Q: The Affordable Care Act (ACA) expanded health insurance coverage to a broader population. What are you hearing about coverage in health insurance exchanges, in particular access to asthma medicines?
A: Some concerns relate to understanding the various plans and how the benefits and coverage applies to asthma medications and treatments. We are hearing questions about formularies, co-pays, co-insurance and deductibles. People need access to the medications that can help them so selecting the “right” plan is important. For example, if people do not choose carefully, they may find that they face a very high deductible or that the medication that they need is not on the formulary.
Q: What are the biggest concerns facing patients with asthma in health exchanges?
A: People want to be able to understand which medications and treatments are available and appropriate for them and their unique circumstance. So, having information in “plain language” that is accessible, understandable and usable to them is important.
Q: Is there anything else we missed?
A: It is very important that people with asthma have access to the medications they need. We worry that this will be more challenging and might become even more contentious, as innovative yet often costly medications (such as biologics and 3D printed products) emerge from pharmaceutical pipelines. We think it is critical to introduce these important innovations in a way that assures that the patients who need them will have access to them, while assuring that they are available and affordable to patients. What is needed is a better understanding of what works, what works best, and for whom. To do so will require much more dialogue among various stakeholders including payers and the pharmaceutical industry. AAFA believes that such dialogue has to begin with the question: what is best for patients?
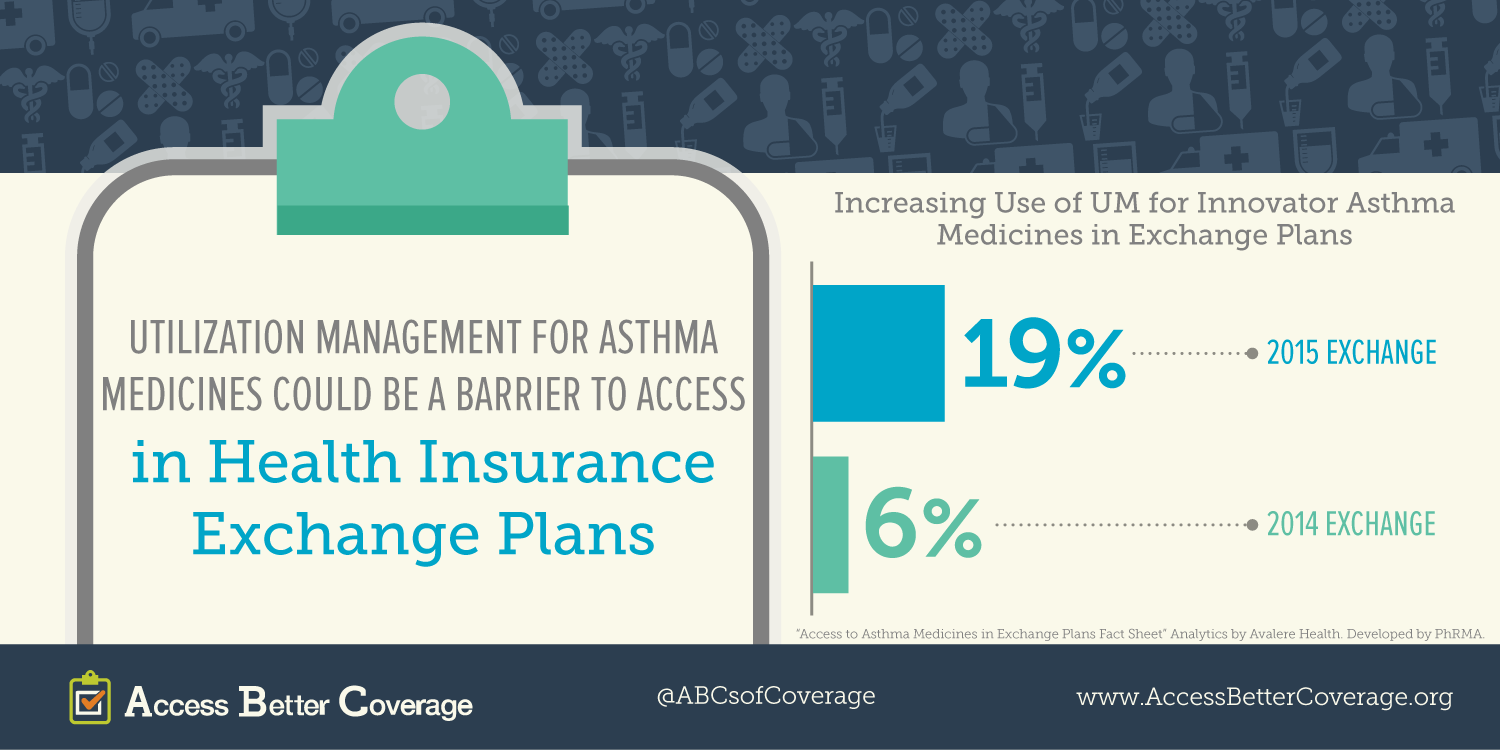



 Q: The Affordable Care Act (ACA) expanded health insurance coverage to a broader population. What are you hearing about coverage in health insurance exchanges, in particular access to asthma medicines?
Q: The Affordable Care Act (ACA) expanded health insurance coverage to a broader population. What are you hearing about coverage in health insurance exchanges, in particular access to asthma medicines? 