Recently, we discussed the obstacles patients face in managing chronic conditions such as mental health disorders, HIV/AIDS and Rheumatoid Arthritis under the Affordable Care Act’s health insurance exchanges. Patients face many challenges in accessing the medicines they need, but the burden on patients increases with the complexity of the disease.
As a result, those with Multiple Sclerosis (MS) are at a disadvantage. The autoimmune inflammatory disease of the central nervous system is incredibly complex and affects each patient differently, making it difficult to treat because it takes several forms. Years of research has led to the development of innovative new medicines that play a vital role in the long-term management and prevention of the disease’s progression. The development of these treatments is critical because successfully treating MS is not a one-size-fits-all approach.
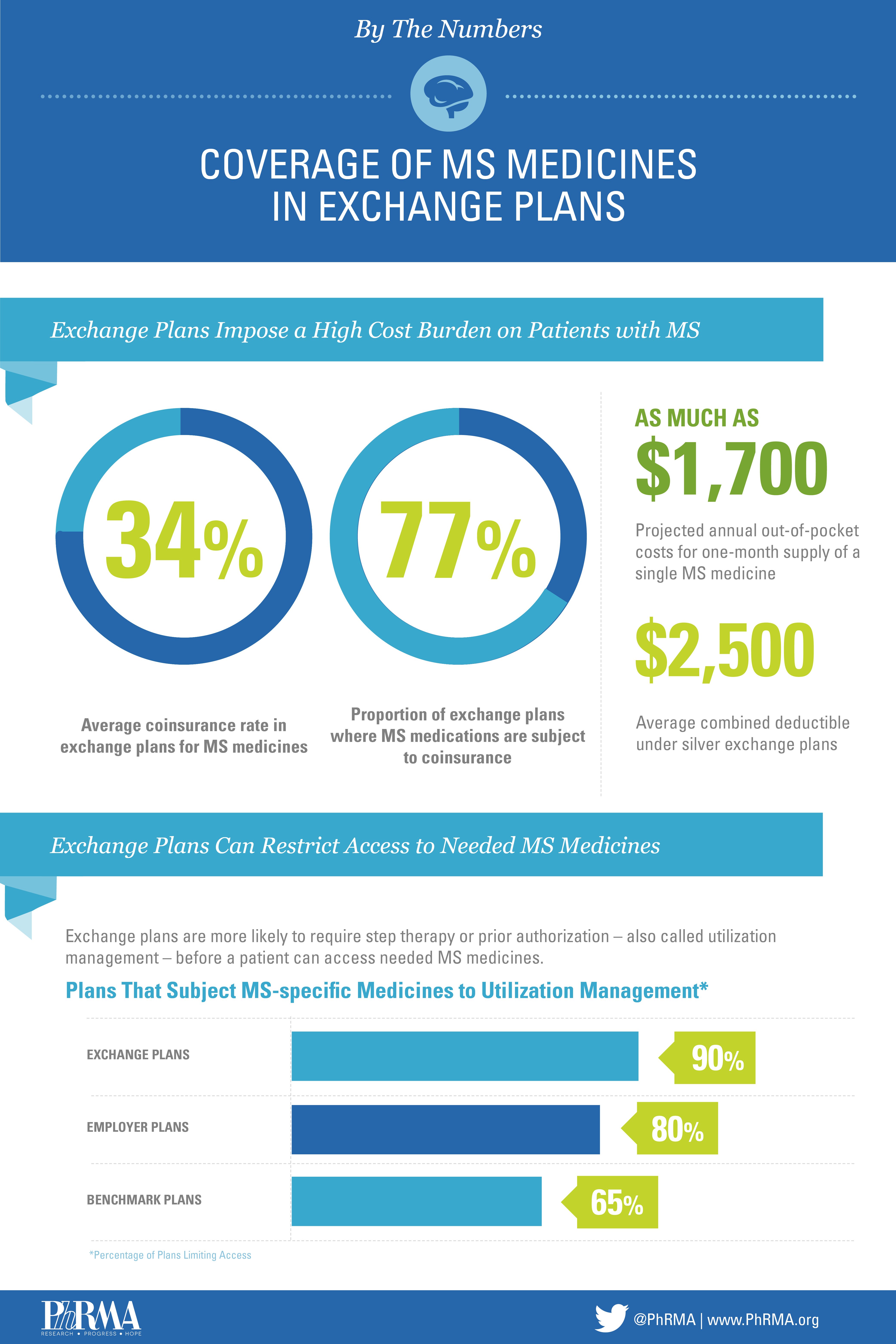
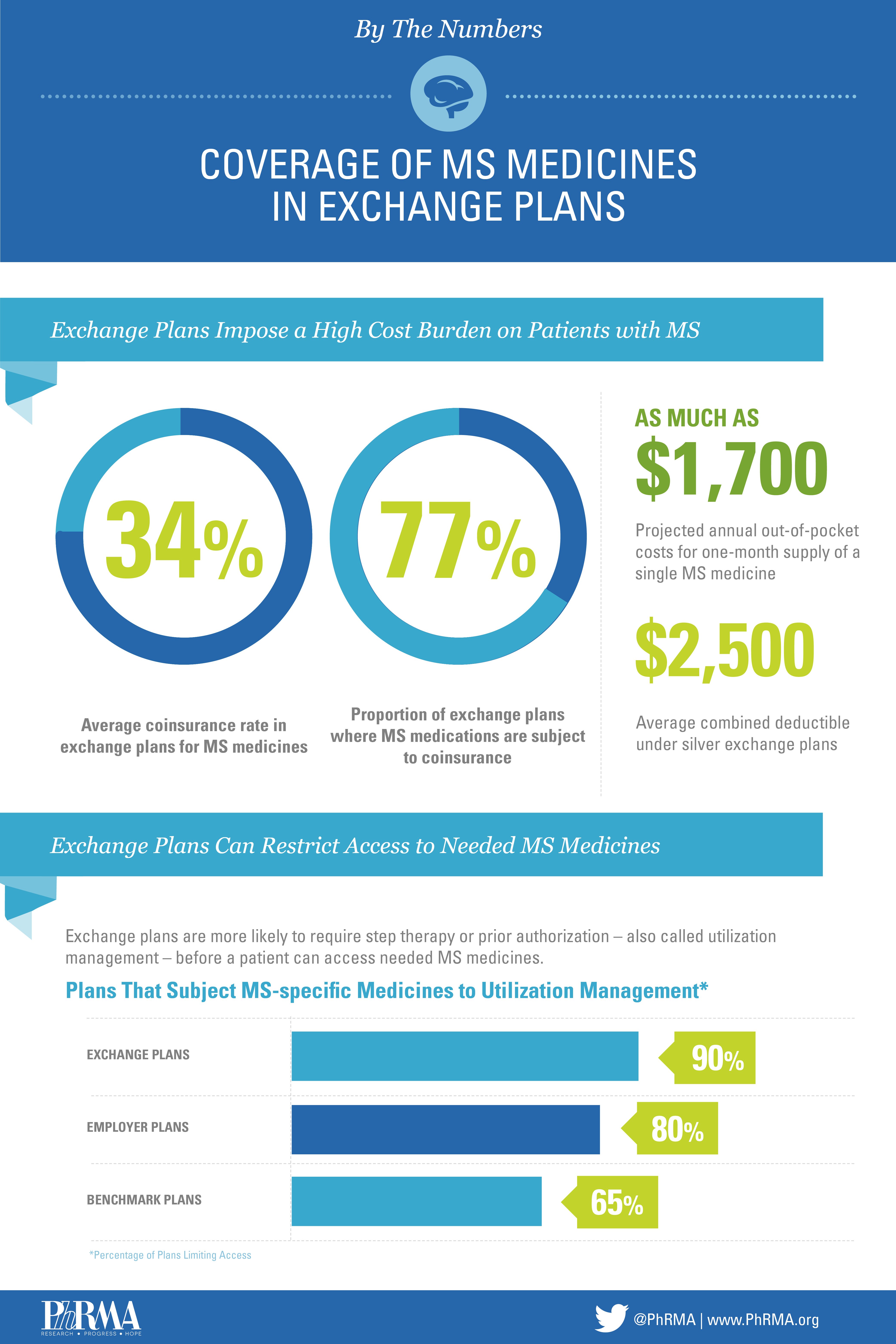
Unfortunately, some health insurance exchange plans are imposing this type of coverage on patients. By requiring high out-of-pocket costs for MS treatments, even when they have a generic alternative, the exchanges are limiting options for individuals and preventing them from effectively managing their condition. In fact, approximately 66 percent of plans put all MS medicines on the highest tier, leaving patients with no lower-cost alternative.
Recent research suggests that approximately 75 percent of silver exchange plans require patients to pay 34 percent of the cost of their prescription medicines. This means an individual could pay as much as $1,700 for a one-month supply of a single prescription. Being able to afford the most effective treatment is essential, but high out-of-pocket costs and a lack of alternatives, results in forgone or inadequate treatment.
As we examine the cost of innovative new medicines, it is also critically important to consider the value they provide patients. Looking solely at the near-term cost often means overlooking the long-term benefit to patients and the health care system. This is especially true for complex diseases like MS. Insisting on a one-size-fits-all model for the treatment of a condition that takes so many forms means increased hospitalizations and more costly care in the future. Virginia Ladd of the Autoimmune Related Diseases Association (ARDA) highlighted this point stating, “The expensive drugs are so beneficial to [patients], they can actually decrease their health care costs, but many didn’t realize when they were signing up [that] they didn’t have a way of determining how that would impact them cost wise.”
As discussions continue regarding how we can help patients access the medicines they need to live longer, healthier lives, we encourage you to follow us on The Catalyst, Twitter and Facebook for more information.