In the last 20 years, medical advances have transformed the lives of Rheumatoid Arthritis (RA) patients. Instead of managing symptoms, innovative medicines help slow disease progression and can even lead to disease remission. Today, patients treated with a combination of both new and older medicines have a 50 percent chance of complete clinical remission after just one year, compared to 28 percent of those taking only older medicines.
This ‘new normal’ for individuals with RA has created incredible value by preventing disability and disfigurement. Unfortunately, access to these medicines is in jeopardy.
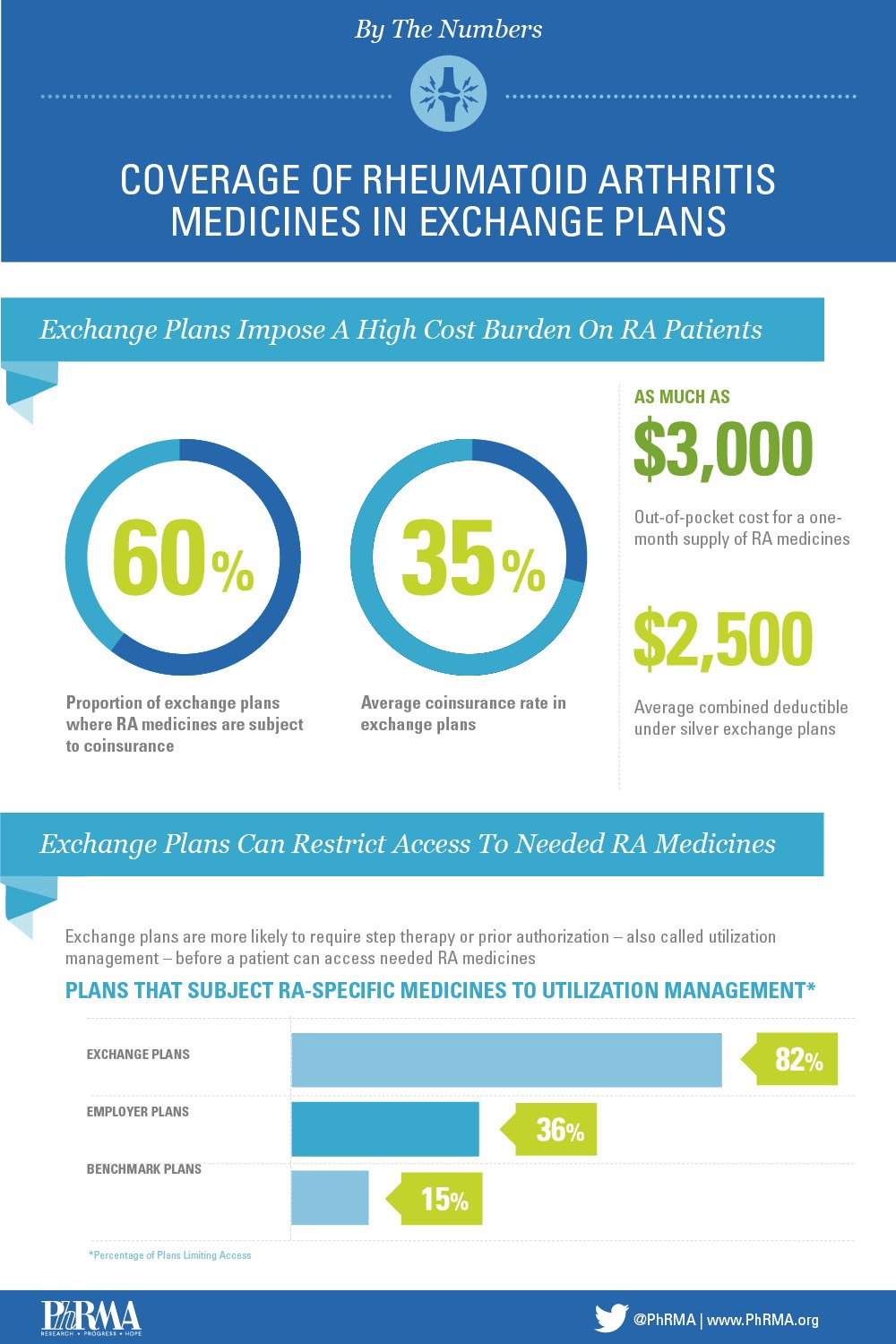
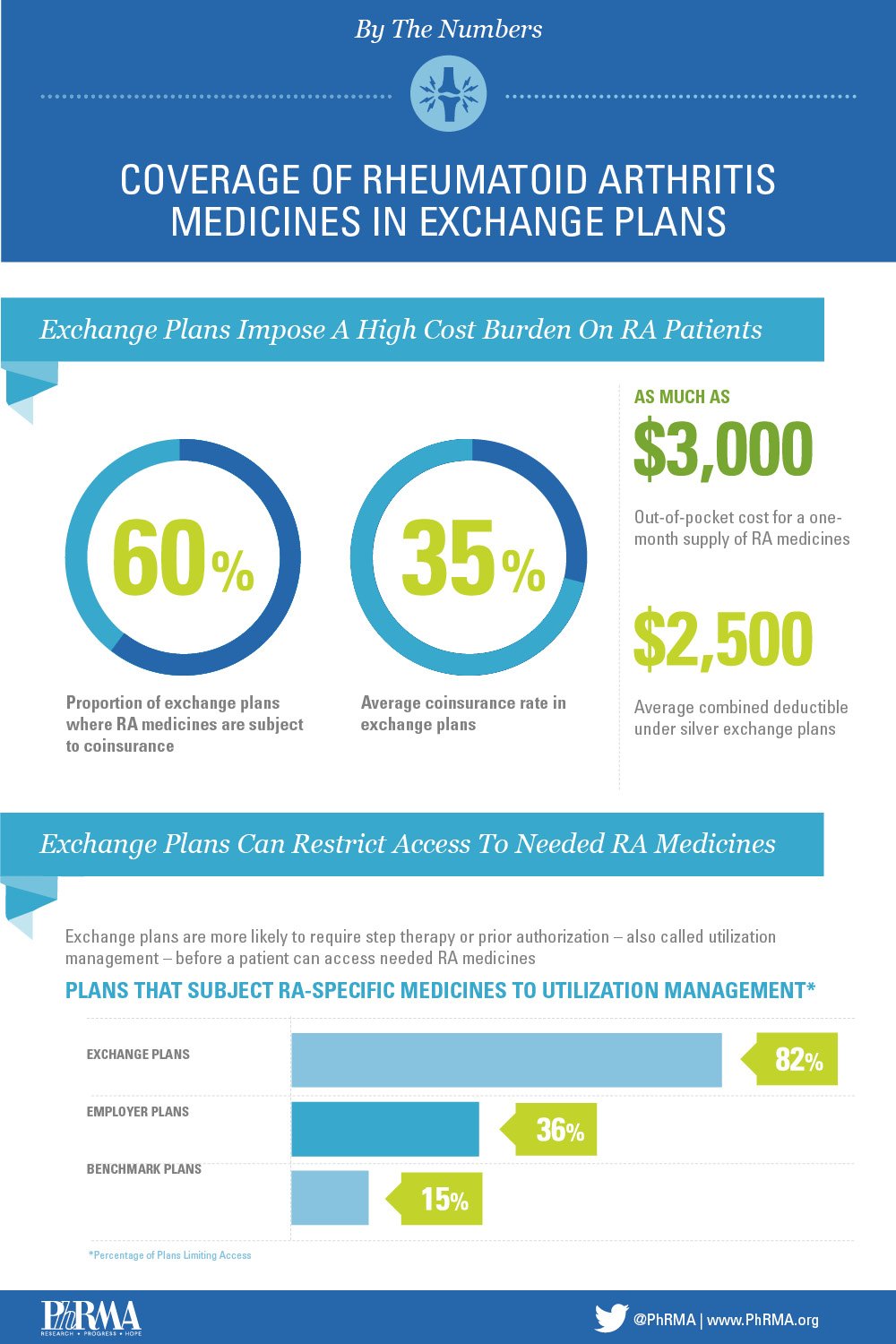
The health insurance exchanges in the Affordable Care Act were intended to help patients get the treatments they need. While the exchange plans cover many RA-specific medicines, many of these plans have a single deductible for both prescription medicines and other services. This means that before the cost of any treatment is covered, including prescription drugs, a patient must pay an average of $2,500 or $4,300 out-of-pocket. This makes medicines unaffordable for patients and significantly increases the chances of non-adherence.
More shocking is the exorbitant cost-sharing required for the medicines RA patients rely on to treat and manage their condition. Nearly 60 percent of the time, RA medicines covered by exchange plans are subject to 35 percent coinsurance. This means that a patient may face high cost-sharing – as much as $3,000 for a one-month supply for a single medicine to treat their condition – a cost many patients may be unable to afford.
Dr. William Harvey of the American College of Rheumatology and his colleagues have seen this first-hand. In an example he shared when testifying before the House Energy and Commerce Committee, Dr. Harvey told the story of a young mother in her 30s whose high copays and deductibles mean she cannot afford the advanced treatments she needs to effectively treat her disease. Instead, she is taking medicine to control her symptoms, and her doctor has “watched RA erode her joints without being able to help.” The disease has already “limited the activities she can do with her children,” and her doctor is concerned that this will eventually affect her employment.
The specific choice of therapy for individuals with RA depends on the severity of the disease when treatment begins and the response to prior interventions. Failing to receive the appropriate medicines not only means the joints are affected, but also impacts other organs including the skin, eyes, lungs and blood vessels, which makes it increasingly difficult to perform normal tasks and maintain employment. “The most vulnerable patients are bearing the cost burden,” says Virginia Ladd, President and Executive Director of the American Autoimmune Related Diseases Association.
It is essential that we take advantage of the most effective treatments available because it not only creates a ‘new normal’ for patients that means longer, more productive lives, but it also means a more effective health care system. As PhRMA’s President and CEO John Castellani noted a few weeks ago, “It is penny wise and pound foolish to focus solely on the price of a new medicine while completely ignoring the value it provides to patients and the health care system more broadly.”
Be sure to follow us on The Catalyst, Twitter and Facebook for more and check out our new fact sheets on what the exchanges mean for patients suffering from chronic conditions.