There is only one place in the health care system where middlemen refuse to share negotiated prices with patients, and that’s at the pharmacy counter. A new report reveals how this harmful tactic leads to higher costs for patients.
Health insurers and pharmacy benefit managers (PBMs) negotiate rebates and discounts that lower the price they pay for prescription medicines. The problem is they don’t always share these lower prices with patients who rely on prescription medicines.
Instead, a patient in their deductible shows up at the pharmacy and is required to pay the full list price of the medicine. Insurers and PBMs also require patients with coinsurance to pay based on the full price of the treatment by charging them a percentage of the medicine’s full list price.
A new report, based on an IQVIA analysis of health care spending data of commercially insured patients taking brand medicines, shows how these tactics are increasingly shifting the cost of medicines to patients. Here are three key facts from this new report:
Fact #1: Patients with deductibles and coinsurance face higher costs at the pharmacy.
Insurers and PBM’s increasing use of deductibles and coinsurance is sticking patients with higher out-of-pocket costs at the pharmacy — significantly higher costs. The data show that patients with deductibles or coinsurance spent six times more out of pocket for their medicines per year than patients who only had to pay a simple, flat copay.
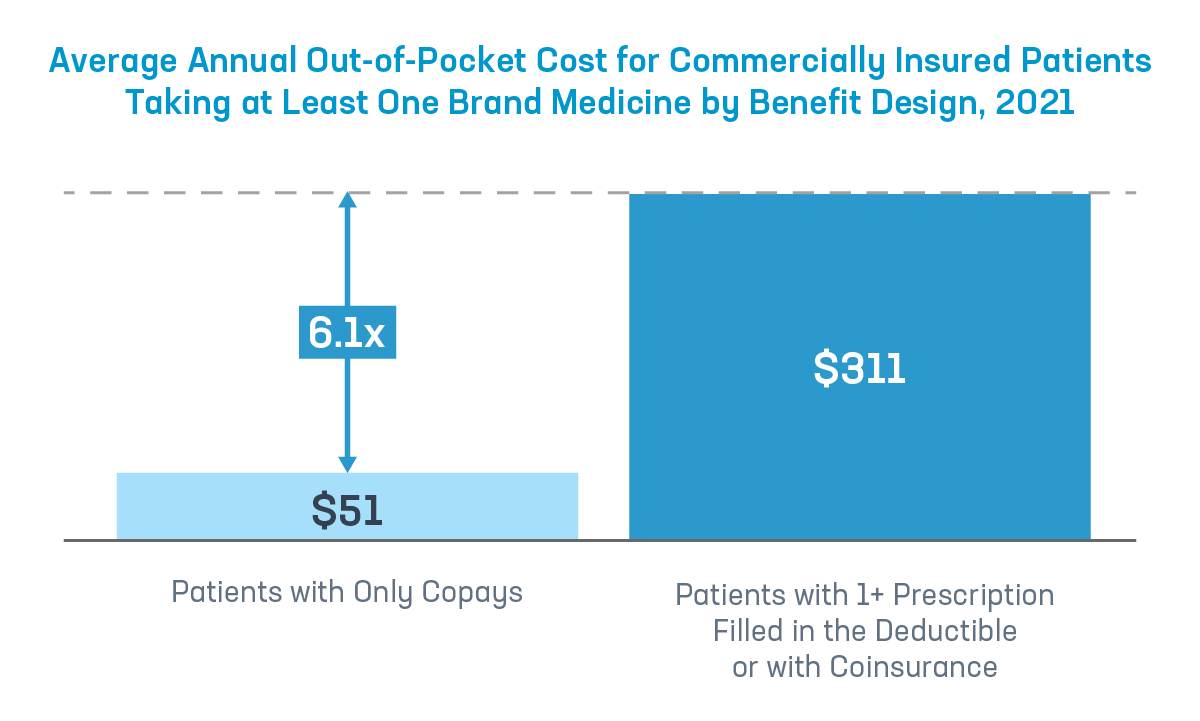
Fact #2: Shifting costs to patients can lead to harmful consequences.
When out-of-pocket costs go up, the chances that patients will take their medicines goes down. In fact, patients are almost four times more likely to abandon a new brand prescription when filled in the deductible compared to one filled with a flat copay. The rate of abandonment is also higher for patients paying with coinsurance also. Research has shown that patients who abandon their medicines experience worse health outcomes.
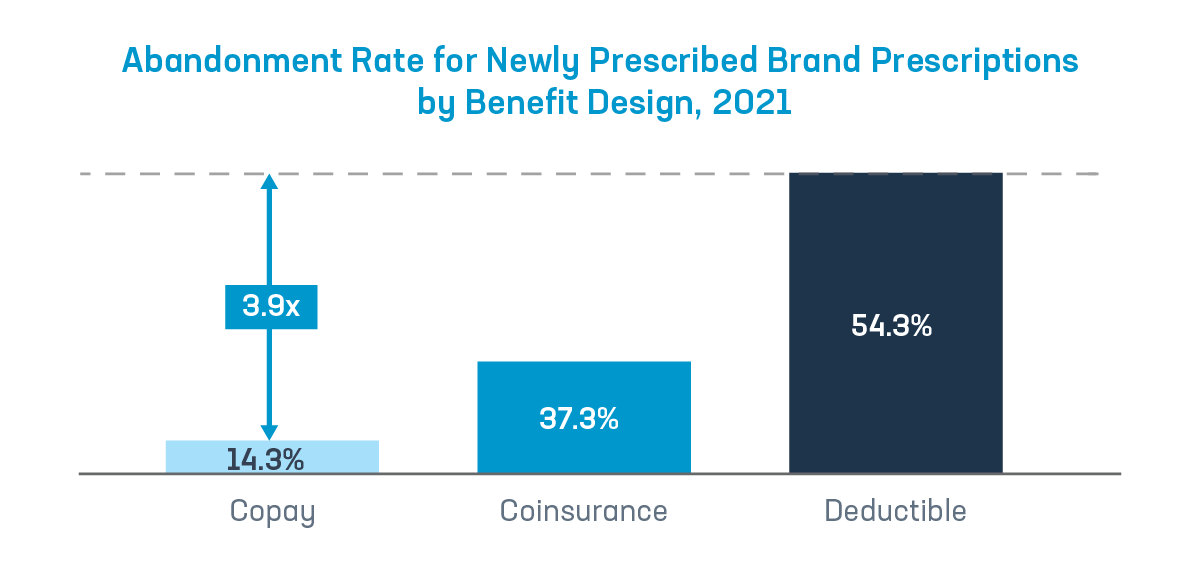
Fact #3: Patient assistance provides a vital lifeline.
As insurance coverage has eroded over time, biopharmaceutical companies have stepped up to help. Many now offer various forms of patient assistance — such as copay coupons — that help patients afford their out-of-pocket expenses. And this patient assistance can make a real difference.
The report shows that patients with commercial insurance using this type of assistance saved an average of $498 per year on their prescription medicines. But now insurers and PBMs are using various schemes to cut this vital lifeline.
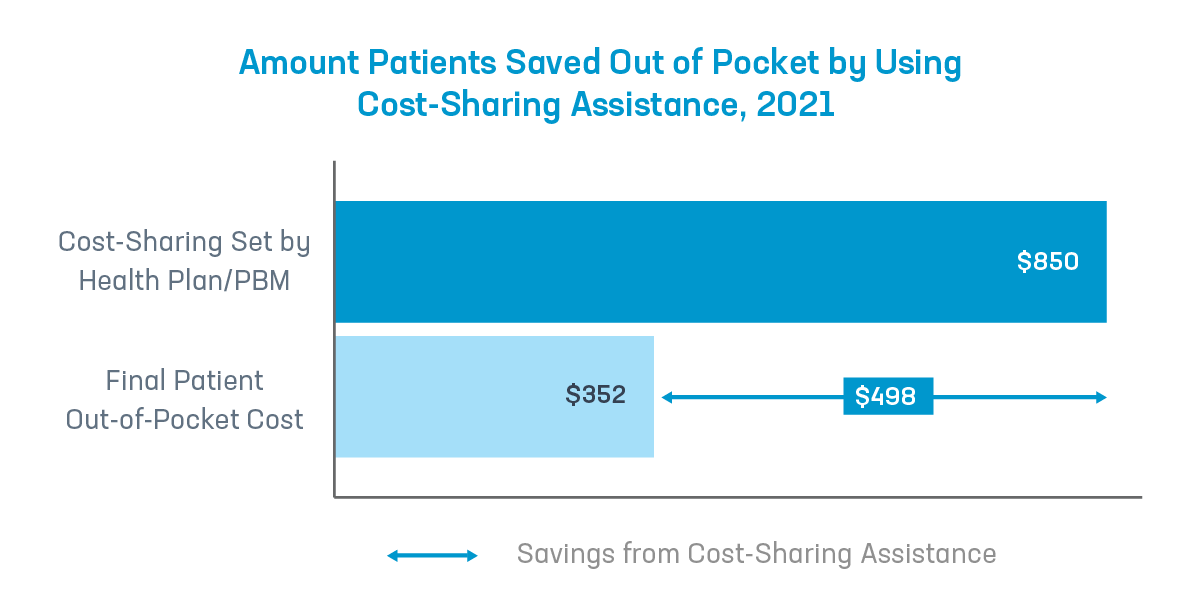
Making the system work better for patients.
In today’s health care system, insurers and PBMs exploit patients who need lifesaving medicines. Fortunately, there are some simple steps policymakers can take that would bring immediate relief to patients.
For starters, let’s make sure that what patients pay out of pocket for medicines isn’t more than what insurance companies pay. We need to ensure that patient with deductibles and coinsurance receive the lower, negotiated price their health plans pay.
And let’s stop tactics by insurers and PBMs that deny people who can’t afford their medicines the benefit of patient assistance support. Patient assistance support doesn’t cost health plans and middlemen a dime, but can be invaluable to someone who can’t afford their treatment. Let’s make sure patients who are eligible for assistance can get the help they need.
To learn more about insurers and pharmacy benefit managers, visit PhRMA.org/Middlemen.
Read the one-pager here and the full report, click here.






