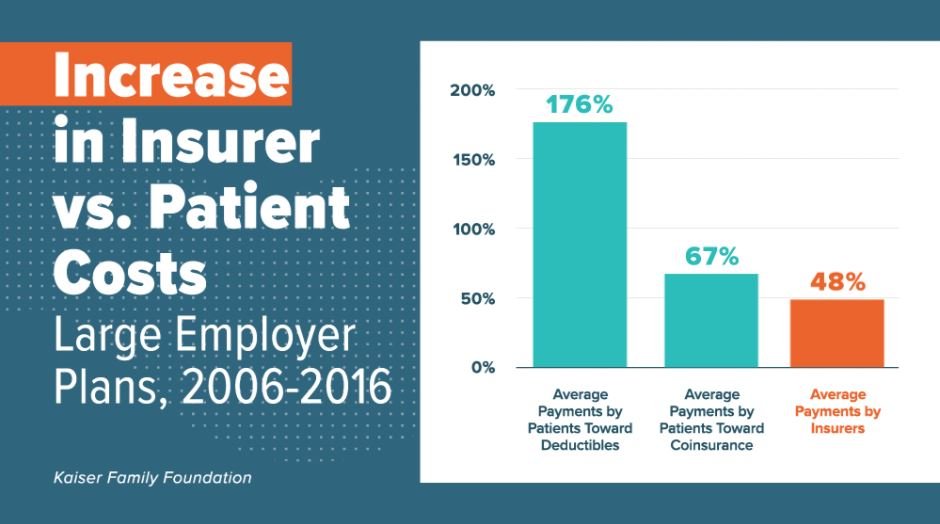
Newly released data from the Kaiser Family Foundation show out-of-pocket costs for patients with employer-sponsored health insurance rose faster than the costs paid by their insurers between 2006 and 2016. Over this decade, the total amount patients spent out of pocket grew, on average, from $525 to $806. That increase of 54 percent is higher than the increase in payments by health insurers, which rose 48 percent, on average, over the same time period (from $3,182 to $4,724).
In addition, from 2006 to 2016:
- Average patient payments toward deductibles rose from $151 to $417, an increase of 176 percent.
- Average patient payments toward coinsurance -- a percentage of costs a patient is responsible for paying out of pocket -- rose from $149 to $249, an increase of 67 percent.
- Average patient payments toward copays – a fixed cost – decreased 38 percent from $225 to $140.
As patient out-of-pocket costs increase dramatically and cost-sharing shifts from fixed copays to less predictable deductibles and coinsurance, patients will continue to face affordability challenges. Even though rebates paid by biopharmaceutical companies often substantially reduce what insurers and pharmacy benefit managers (PBMs) pay for medicines, insurers typically use list prices—rather than discounted prices—to determine how much to charge patients with deductibles and coinsurance. In 2017, more than half of patient out-of-pocket spending for brand medicines was for prescriptions filled in the deductible or with coinsurance. No patient should pay more for their medicine than their insurer.
Learn more at LetsTalkAboutCost.org.




