Today, we released the results in the first report in a series on patient experiences with the health care system. The report, titled “Barriers to Health Care Access in the Patient Experience,” surveyed over 4,700 Americans to explore the barriers they face in access to health care and prescription medicines.
The survey revealed that 3 in 10 Americans that have insurance still face a financial barrier to care, like having trouble paying medical bills or having out-of-pocket costs that are more than they can afford. Health insurance just isn’t working like it should because insurers and pharmacy benefit managers are increasingly shifting more health care costs onto patients through high deductibles and coinsurance.

Health insurance benefit design and out-of-pocket costs are barriers to care that can lead to nonadherence (when a patient does not take their medicines as prescribed by their doctor). The study found:
- Half of patients (52%) with a high-deductible health plan reported an episode of nonadherence in the past year, meaning they had trouble taking their medicines as prescribed.
- 87% of Americans with medical debt experienced nonadherence issues in the past year alone.
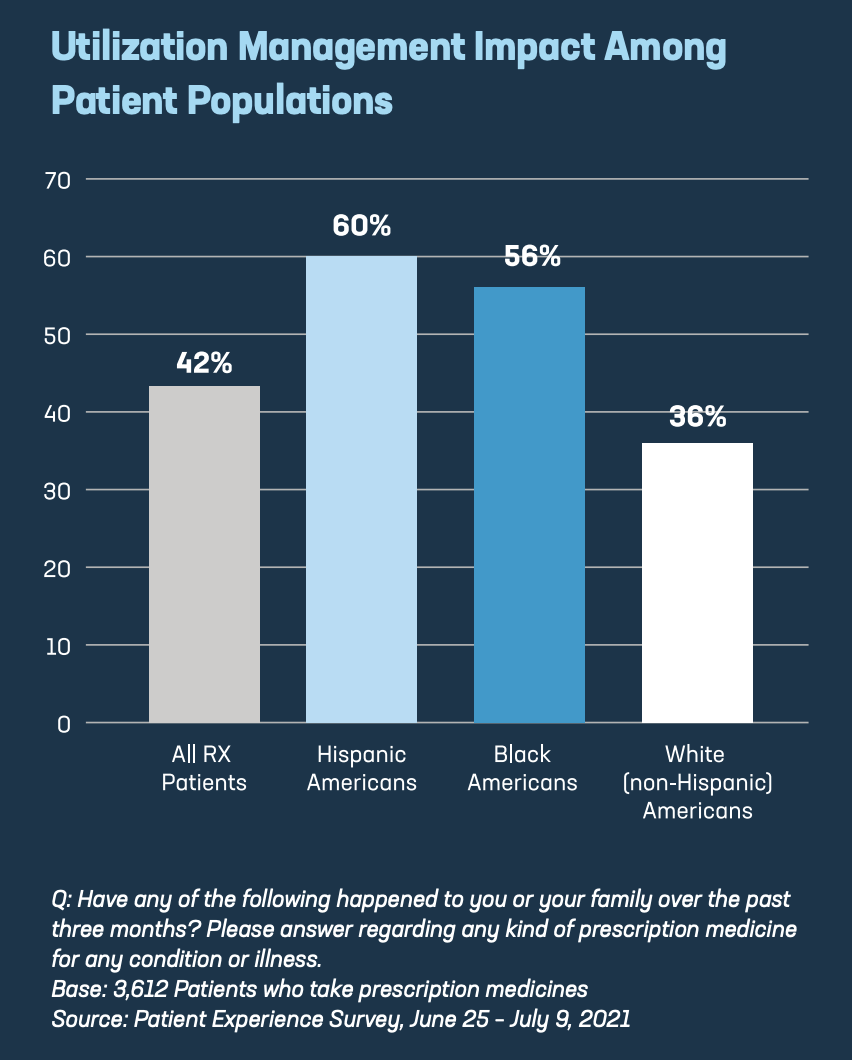
The study also found insurer practices like utilization management – including prior authorization and step therapy – are more likely to affect the sickest and most vulnerable in our health care system. These findings include:
- Patients with some of the most serious chronic diseases – autoimmune diseases (62%), allergies (52%) and diabetes (52%) – are more likely to report experiences with utilization management than other Americans who take prescription medicines.
- While majorities of Black Americans (56%) and Hispanic Americans (60%) report being subjected to utilization management practices, only 36% of white Americans report experiencing the same.
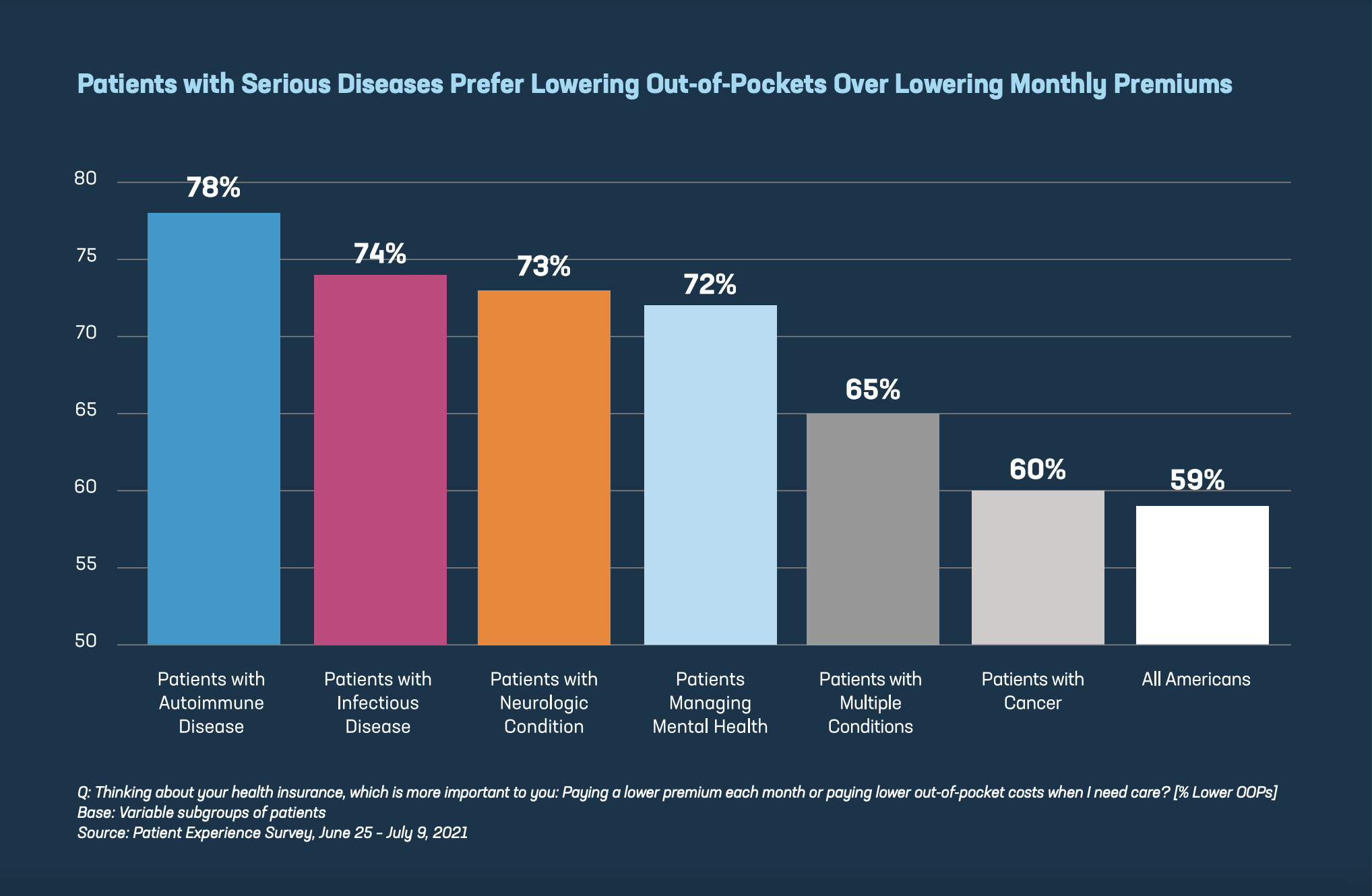
To fix these issues, 59% of patients prioritize lowering their out-of-pocket costs, not their premiums (41%). Other recent polling shows a drastic decline in public support by as much as 51 points, overall, for letting government set prices for medicines once Americans learn more about this policy. In particular:
- Only 15% support when told it could limit people’s access to newer prescription medicines;
- Only 15% support when told that taxing medicines up to 95% for non-compliance could take money out of the search for new medicines and cures; and
- Only 16% support when told it could lead to less research and development of new medicines.
With 40% of Americans reporting COVID-19 has made them more worried and anxious about their family’s ability to access care, policymakers should look at the entire health care landscape and patient experience to improve the health care system.
Read the report here and learn more about patient-centered solutions at PhRMA.org/BetterWay.






