More than half of total spending on brand medicines went to the supply chain, middlemen and other stakeholders in 2020 according to a new analysis from the Berkeley Research Group (BRG). These new findings help illuminate the problems that exist throughout the health care system and why holistic, patient-centered solutions are needed to make medicines more affordable for patients.
The analysis looks at all spending on brand medicines at the pharmacy or paid on a claim to a health care provider. Here are three things from the analysis that you should know:
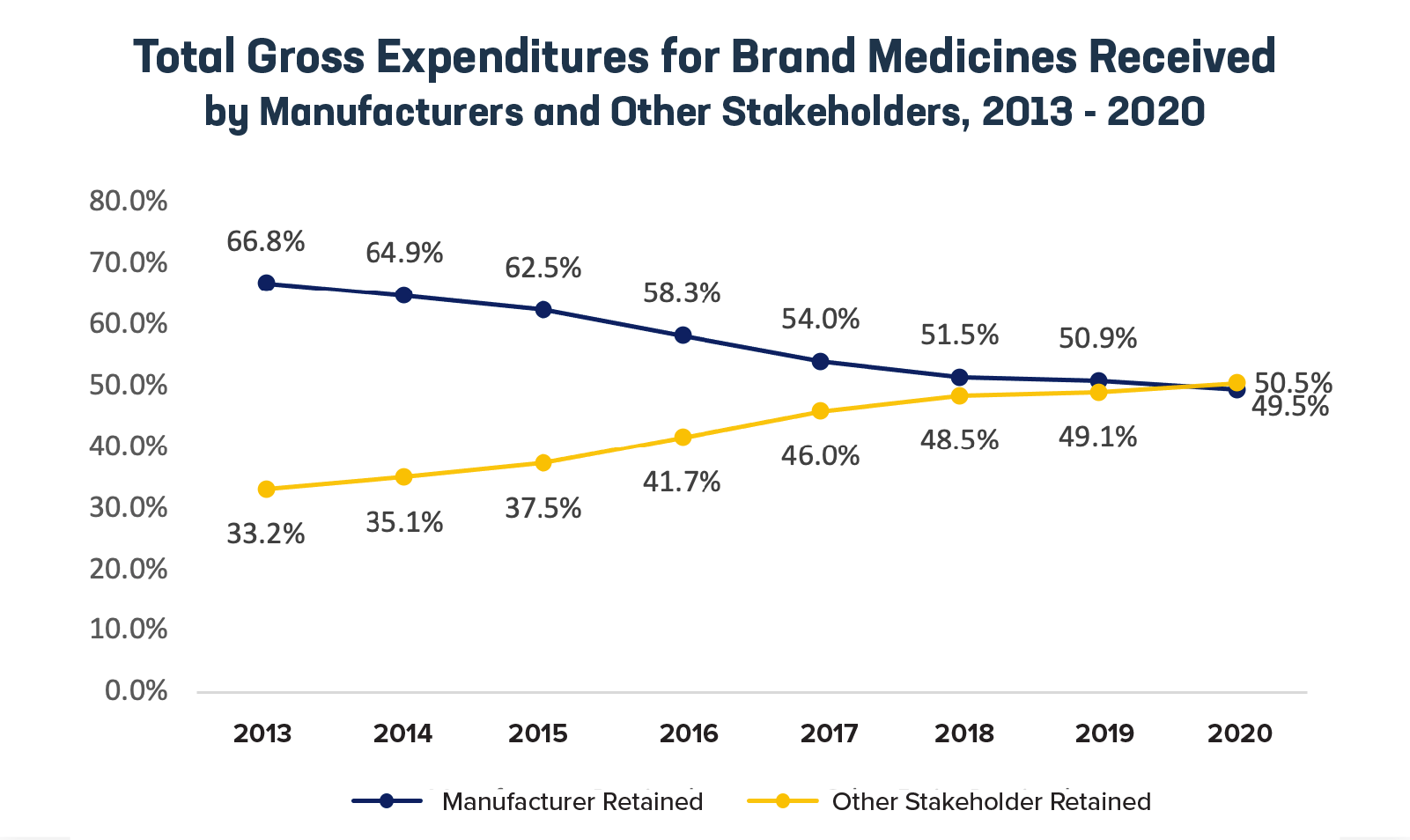
1. More than half of every $1 spent on brand medicines went to payers, middlemen, providers, and other stakeholders in 2020. For the first time since BRG began tracking trends in pharmaceutical spending eight years ago, the share of brand medicine spending retained by biopharmaceutical companies has fallen to less than half (49.5%) of total spending.
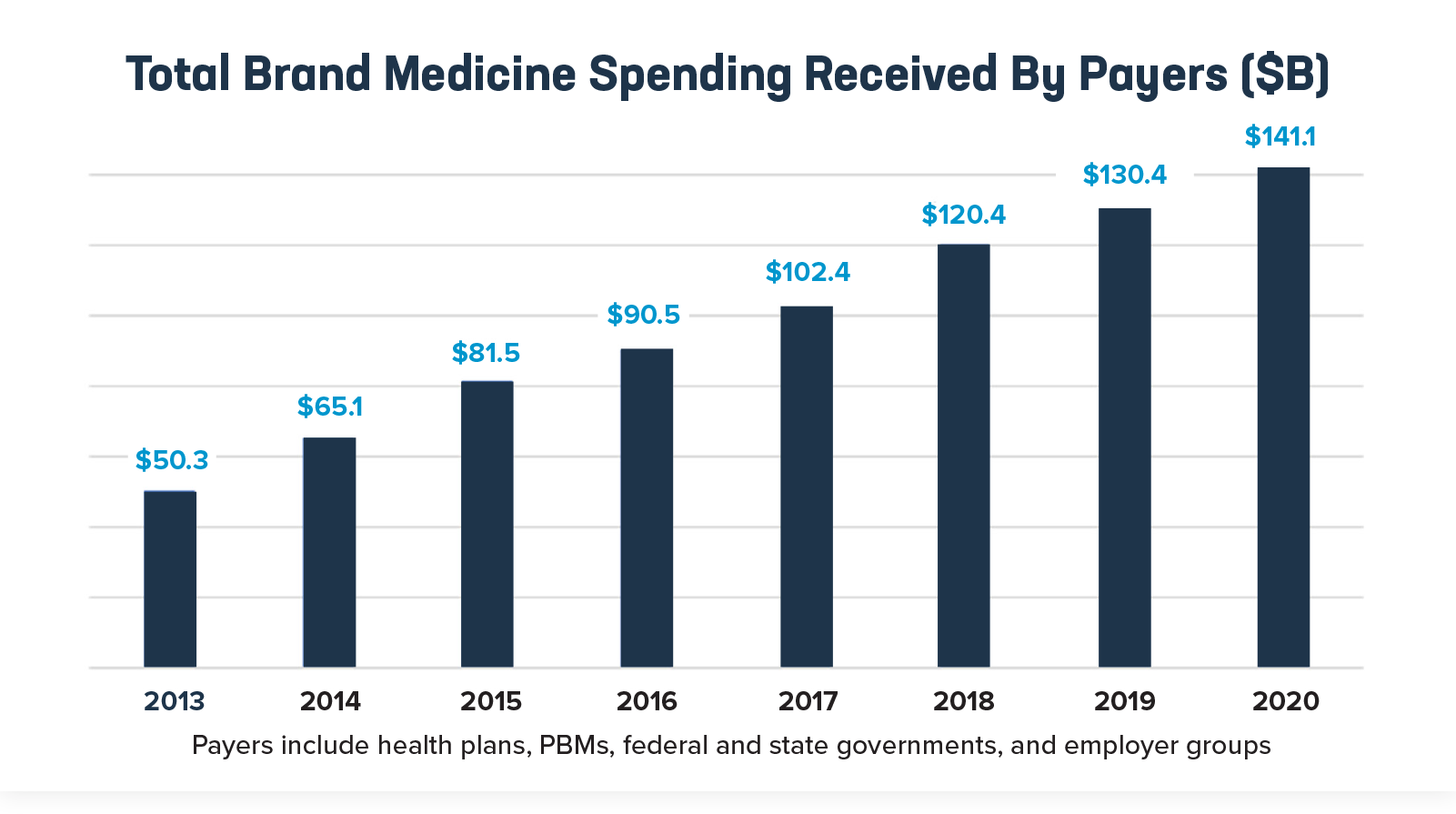
2. Payers, including insurers, PBMs and government programs, received more than $140 billion in spending on brand medicines. This spending reflects rebates, discounts and other payments from biopharmaceutical companies that lower the cost of medicines. However, savings in the system are often not shared with patients at the pharmacy counter.
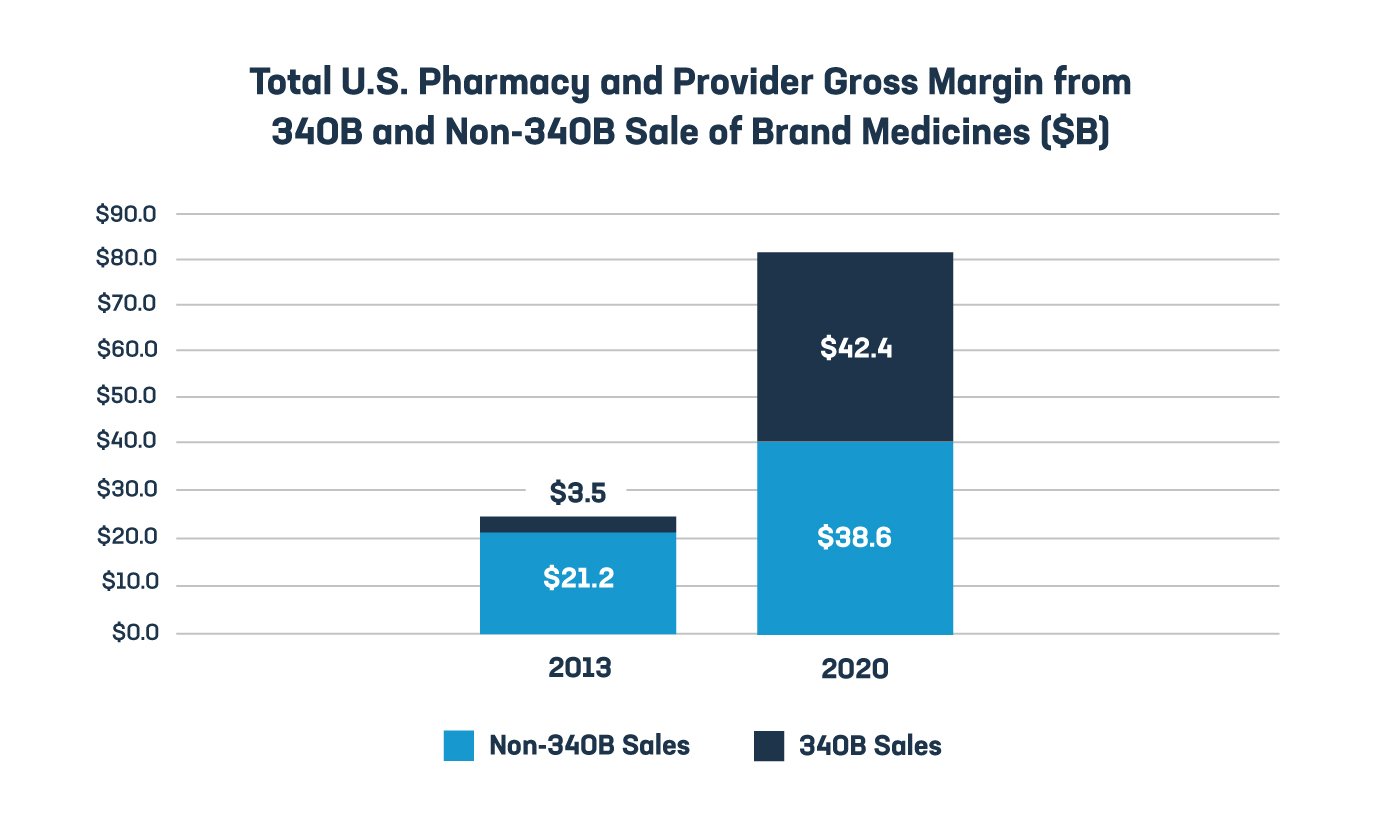
3. Unprecedented growth of the 340B drug pricing program resulted in a 1,100% increase in the amount hospitals and other 340B entities received from the sale of brand medicines purchased through the 340B program between 2013 and 2020. During that same time period, over 94,600 contract pharmacy relationships were established, contributing to the growth in 340B pharmacy and provider margins on brand medicines.
America’s biopharmaceutical research industry is ready to do its part to deliver a health care system that works better for patients. As PhRMA President and CEO Steve Ubl noted:
“When more than half of what is spent on medicines goes to entities that have nothing to do with making them, the system needs to change. … It’s time that policymakers accurately diagnose the problems that exist across the supply chain and the challenges patients actually experience.”
Ubl went on to say: “We must address what is really driving up costs for patients.”
View the full analysis here. Download a fact sheet on this topic here.






