Two studies released last month reveal how hospitals across the country mark up the price of medicines and deliver a growing share of provider-administered medicines, resulting in higher costs that are often passed onto patients.
- A study published in the American Journal of Managed Care examined the price of care at more than 3,200 hospitals in all 50 states and found substantial charge variation by hospital across oncology services. “What we found in the marketplace is that over one quarter of the medical centers that provide cancer services are charging more than 5.1 times the Medicare allowable amount, and in some cases the centers are charging more than 15 times the Medicare allowable amount,” noted lead author Martin Makary, MD, MPH, a cancer surgeon at Johns Hopkins Hospital. The study found the most significant markups at hospitals with for-profit status for medical oncology services and hospitals with prestige status for radiology and pathology.
- A separate study published by JAMA Oncology showed a staggering difference between the cost of chemotherapy depending on the site of care. The research found that the same care provided in a hospital outpatient department cost roughly double than in a physician’s office for commercially insured patients. For example, the average spending on chemotherapy medicine was $1,466 for treatments administered in a physician’s office, but hospitals receive $3,799 ($2,333 more). Despite the cost disparities, the study also concluded that the delivery of chemotherapy is trending towards hospitals and away from physicians’ offices. In 2004, only 6 percent of infusions occurred in the hospital, compared to 43 percent in 2014.
Provider consolidation and markups increases costs for the health care system and, ultimately, for patients. One key driver of this consolidation is the 340B program, which allows qualifying hospitals to obtain steep discounts for prescription medicines. Current program guidance allows 340B hospitals to extend their 340B eligibility to independent physician practices they’ve purchased. These hospitals can then be reimbursed by commercial payers for medicines administered at these offices at the regular negotiated rate – and pocket any different between their reimbursement and the 340B discounted price.
A recent study in the New England Journal of Medicine concluded that financial incentives created by the 340B program have led 340B eligible hospitals to alter their behavior by acquiring more physician practices and increasing hospital administration of drugs. Congress created the 340B program to support safety net providers, yet the analysis found no evidence 340B hospitals use revenue derived from the program to “invest in safety net providers, provide more inpatient care to low-income patients, or enhance care for low-income groups in ways that would reduce mortality.”
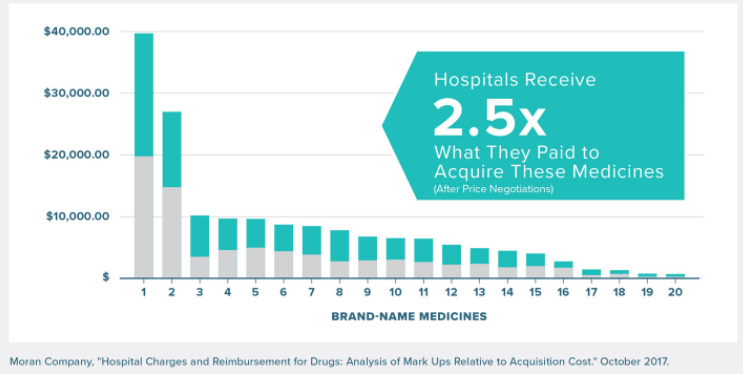
As has been discussed in prior Catalyst blogs, the Moran Company found hospitals receive, on average, more than 250 percent what they paid for a medicine after negotiations with commercial payers, even without accounting for discounts provided through the 340B program. In these cases, a hospital is ultimately paid more than the biopharmaceutical company who brought the medicine to market.
As insurers continue to raise patients’ share of health care spending, and hospitals buy up community physicians, these high prices increase patient costs. For underinsured patients or those who need out-of-network services, the impact can be even greater. Patients, especially those fighting cancer, rarely have a choice in where they receive their care, as the urgency of their diagnoses limits their ability to seek other options.
To learn more, visit LetsTalkAboutCost.org.




