Misaligned incentives in Medicare Part D are increasing costs for seniors with diabetes. While insurers negotiate larger and larger rebates with biopharmaceutical companies each year, seniors continue to pay cost sharing based on the pre-rebated price of their diabetes medicine, rather than the lower negotiated rates.
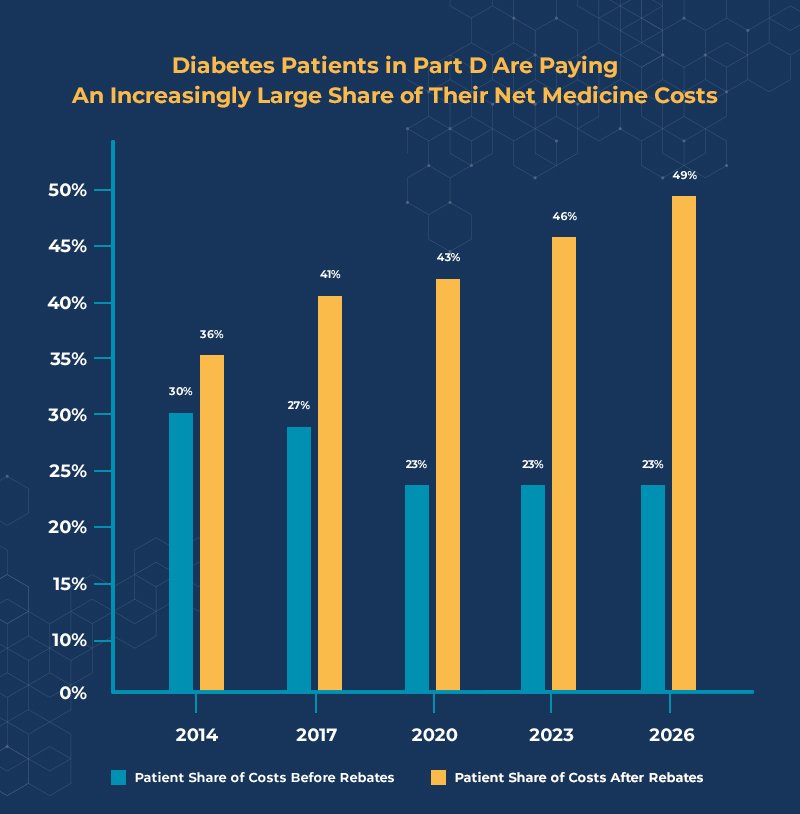
New research by Milliman demonstrates that rebate growth has created a steadily widening gap in the share of total costs paid by Part D beneficiaries on a gross vs. net basis (i.e., before and after rebates are factored in). Part D is structured so that non-low-income beneficiaries pay an average of 25 percent of their pre-rebated medicine costs in the initial coverage phase and coverage gap as of 2020. However, Milliman finds that after rebates, seniors using insulin will pay an average of 46 percent of their medicine costs in the initial coverage phase and 47 percent in the coverage gap in 2020.
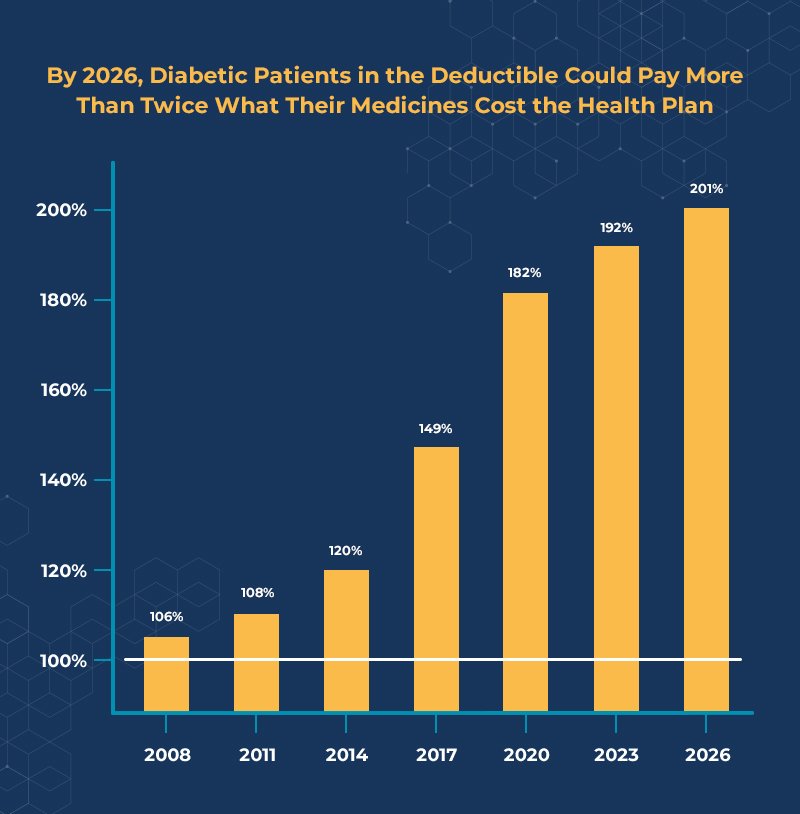
If we don’t reform the rebate system in Part D, diabetes patients could soon pay twice what their insulin and other medications costs to the health plan (the net cost after rebates) when they are in the deductible. In 2008, these beneficiaries paid 106 percent of their net medicine costs in the deductible, but by 2026, that number is projected to almost double to 201 percent. Why should diabetes patients pay twice as much as their insurer for their insulin.
Last fall, the Department of Health and Human Services Office of the Inspector General proposed a regulation encouraging the rebates Part D plans negotiate with biopharmaceutical companies to be entirely passed through to beneficiaries at the pharmacy counter. An analysis by Avalere Health shows that if rebates were used to lower patient costs, a Part D beneficiary taking five medicines, including insulin, could see their annual out-of-pocket spending decrease by $962. Their annual premium could increase by $67, which would result in a total savings of $895. The proposed rule could finally bring down costs for seniors suffering from chronic illnesses.
Learn more about the right solutions to fix Medicare at PrescriptionForMedicare.org.





