According to Kaiser Family Foundation’s recent survey on employer health benefits, premiums for people with employer-sponsored health insurance increased by 4% last year, faster than both the rate of wage growth and inflation. During this same time, prices for brand medicines increased just 1.7% after accounting for rebates and discounts, less than the rate of inflation for the third year in a row.
While medicine prices have remained flat, overall growth in private health care spending still has serious consequences for patients taking medicines, who are also exposed to increasing out-of-pocket costs through coinsurance and deductibles.
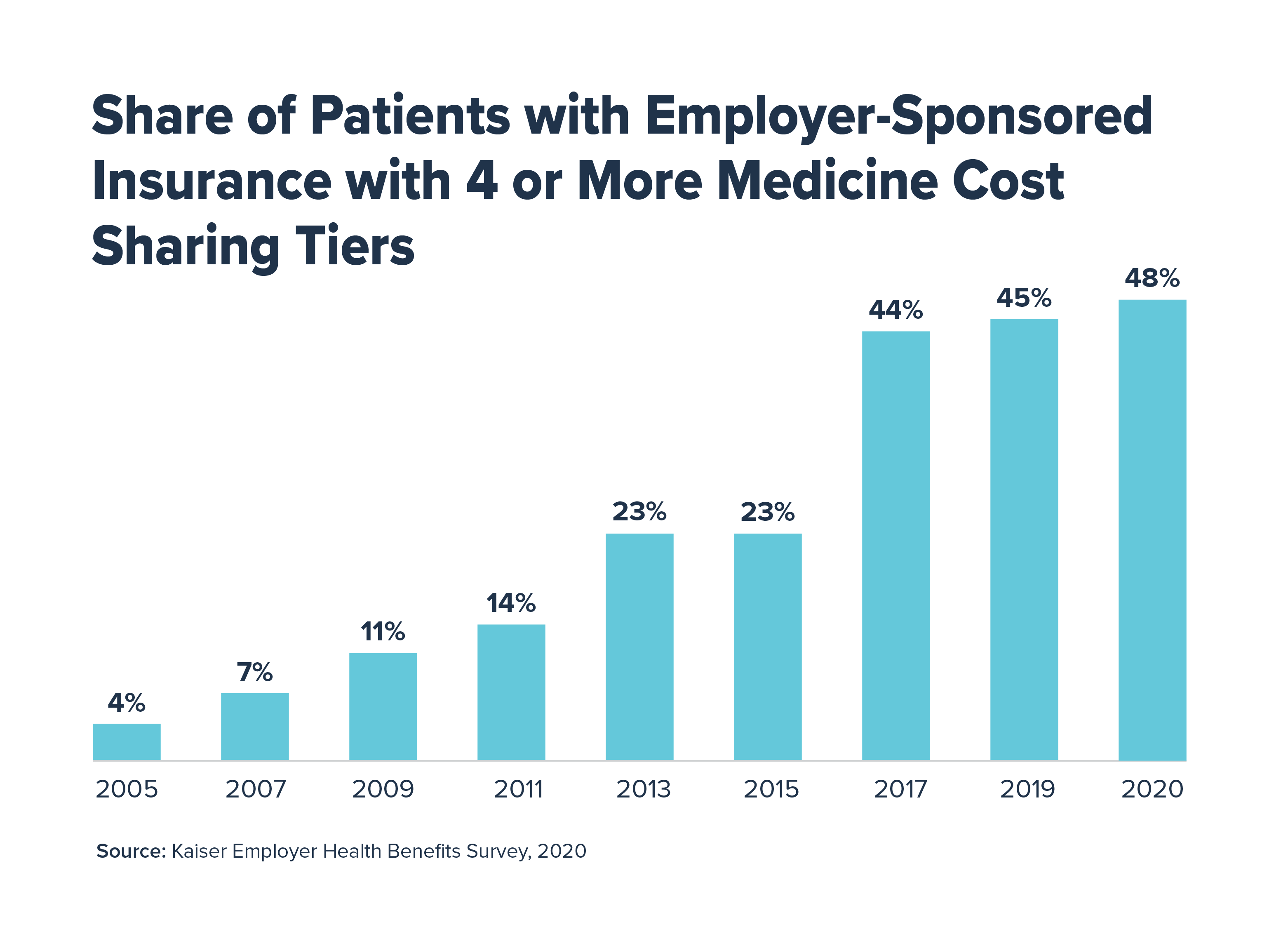
The survey found that this year, 89% of insured workers are in a plan with tiered cost sharing for medicines. Forty-eight percent of workers are in plans with four or more cost sharing tiers, up from just 4% of workers in 2005. Insurers use these tiers to subject certain medicines to higher cost sharing. For medicines on the fourth tier, coinsurance is 28%, on average.
Increasing deductibles are also exposing patients to high out-of-pocket costs. The survey found 83% of workers with employer-sponsored insurance are in a plan with a general annual deductible. On average, this deductible is $1,644 for single coverage, a 25% increase over the past five years and 79% over the past 10 years. For high-deductible health plan enrollees, their average annual deductible for single coverage is $2,303.
Deductibles and coinsurance disproportionately impact patients with complex and chronic conditions who require innovative medicines to manage their health. For example, patients taking brand multiple sclerosis medicines with deductibles or coinsurance spent 32 times more out of pocket annually compared to patients with copays only. This is not how insurance is supposed to work.
We support common sense reforms to fix the system such as lowering patient cost sharing, allowing patients to spread their costs throughout the year and requiring insurance companies and pharmacy benefit managers to share negotiated rebates and discounts with patients. In the meantime, biopharmaceutical manufacturers have stepped up to help patients by providing a broad range of patient assistance in the form of coupons, refund/rebate programs and cost-sharing assistance directly to patients to use when they pick up their medicines at the pharmacy counter.
Learn more at letstalkaboutcost.org.




