 An increasingly popular and alarming trend among 340B hospitals is hurting the integrity of the program and driving up health care costs in the system. Many 340B hospitals are rapidly acquiring independent physician practices then bringing them under the 340B umbrella where they can profit off the “spread” between the 340B price and the reimbursed amount. This trend is helping drive unprecedented program growth and raising health care costs for patients and payers given the more expensive treatment setting. Meanwhile, it’s also reducing patient access to community treatment options.
An increasingly popular and alarming trend among 340B hospitals is hurting the integrity of the program and driving up health care costs in the system. Many 340B hospitals are rapidly acquiring independent physician practices then bringing them under the 340B umbrella where they can profit off the “spread” between the 340B price and the reimbursed amount. This trend is helping drive unprecedented program growth and raising health care costs for patients and payers given the more expensive treatment setting. Meanwhile, it’s also reducing patient access to community treatment options.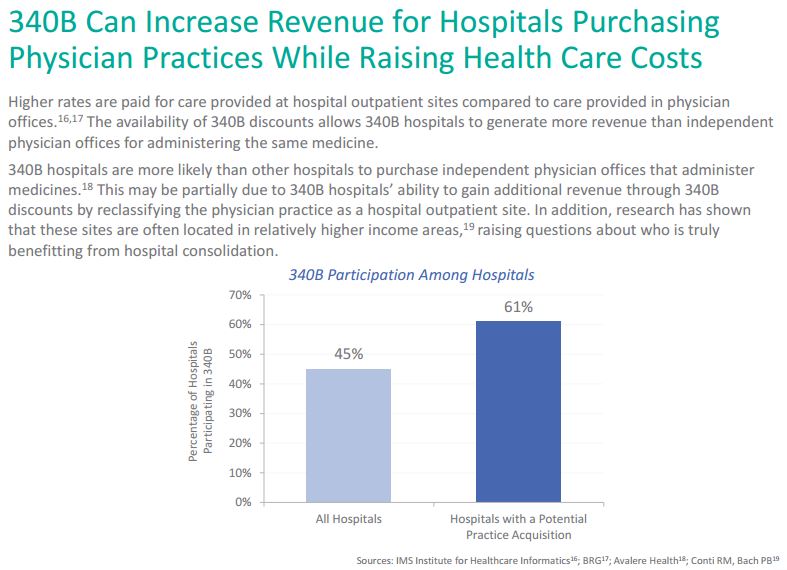
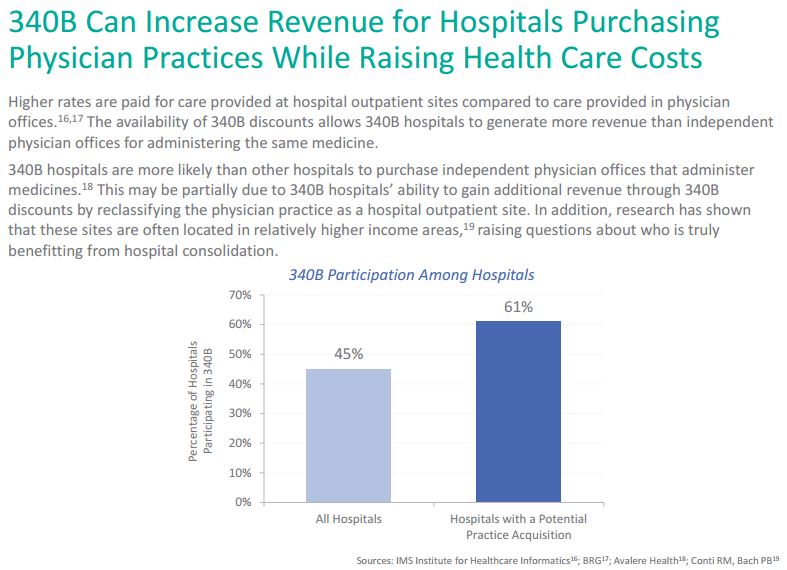
A recent report from Avalere Health shows 340B hospitals are more likely than other hospitals to purchase independent physician offices that administer medicines. Specifically, 61 percent of hospitals acquiring a physician practice are 340B hospitals, even though 340B hospitals make up just 45 percent of the overall set of hospitals included in the study.
This may in part be due to the fact that 340B hospitals can gain additional revenue through 340B discounts by reclassifying the physician practice as a hospital outpatient site, where higher rates for care are paid. However, while the hospital is pocketing extra revenue the discounts the hospital gets are not always seen by the uninsured or vulnerable patients the program was created to help. Mounting evidence also shows these sites are often located in relatively higher income areas, which begs the question of who is actually benefiting from hospital consolidations.
Adding to a growing body of research on 340B hospital consolidation, the Community Oncology Alliance (COA) released a study last week that found much of the growth in the 340B program is concentrated in oncology medicines, which cost Medicare and beneficiaries more when administered through 340B hospitals than at independent physician practices. In fact, the study found the average reimbursement for Part B oncology drugs was 52 percent higher in 340B hospitals than in community cancer clinics, when compared on a per Medicare beneficiary basis. This is concerning given that between 2010 and 2013, 340B hospitals saw a 123 percent increase in total Part B reimbursement for oncology medicines, compared to just 31 percent at non-340B hospitals. At the same time, reimbursement to physician offices declined by 5 percent.
 Check out our chart pack for more information or stay up-to-date on the latest 340B news with our 340B Spotlight posts.
Check out our chart pack for more information or stay up-to-date on the latest 340B news with our 340B Spotlight posts.


 An increasingly popular and alarming trend among 340B hospitals is hurting the integrity of the program and driving up health care costs in the system. Many 340B hospitals are rapidly acquiring independent physician practices then bringing them under the 340B umbrella where they can profit off the “spread” between the 340B price and the reimbursed amount.
An increasingly popular and alarming trend among 340B hospitals is hurting the integrity of the program and driving up health care costs in the system. Many 340B hospitals are rapidly acquiring independent physician practices then bringing them under the 340B umbrella where they can profit off the “spread” between the 340B price and the reimbursed amount. 
 Check out our
Check out our