Concerns about inflation continue to be top of mind for many Americans, as prices for basic services and necessities climb at a rapid pace. But there is one bright spot in this otherwise bleak picture: Between January 2021 and January 2022, prices for prescription drugs only increased marginally and well below the rate of general inflation.
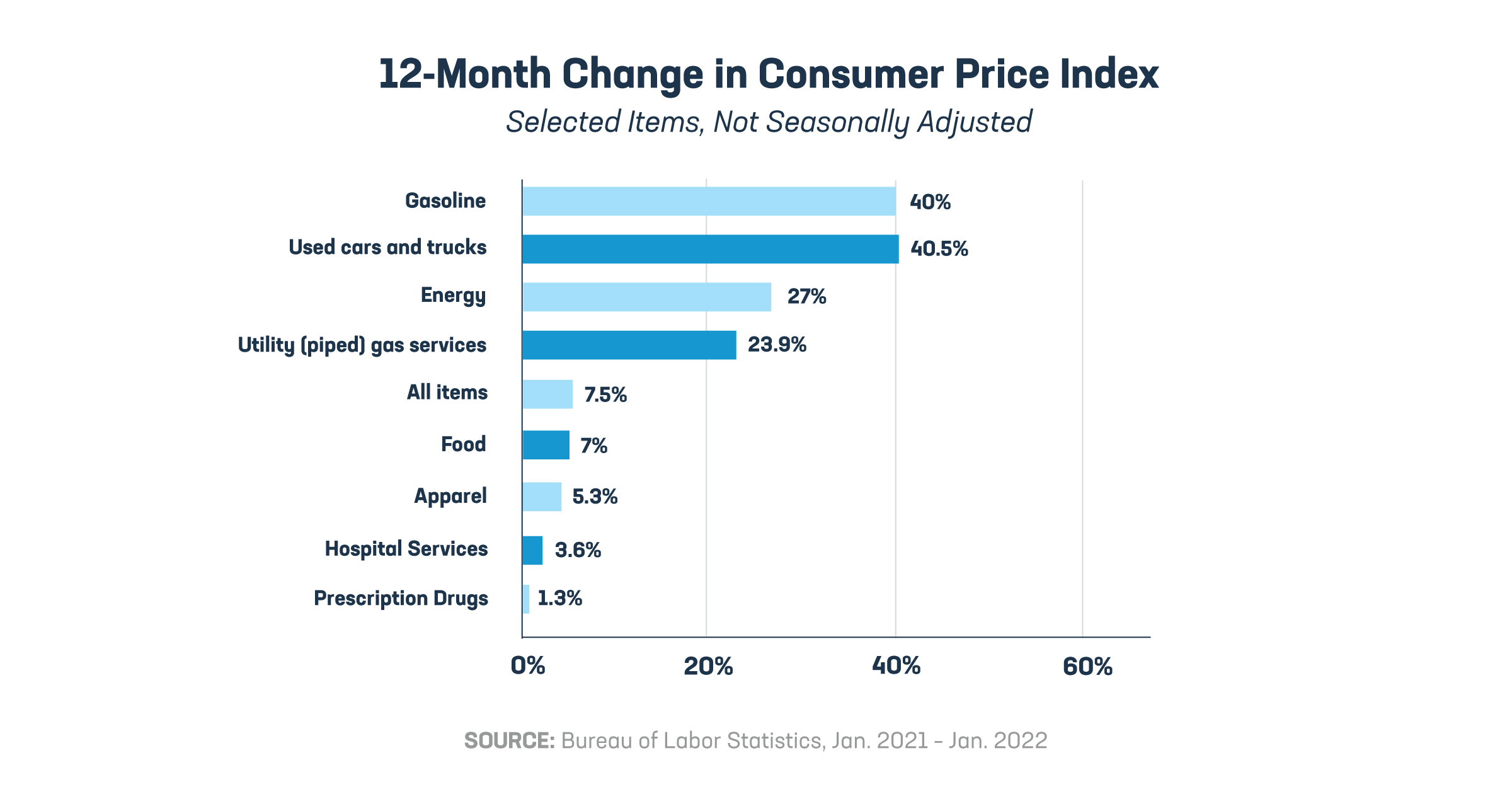
According to the Bureau of Labor Statistics, prescription drug prices rose just 1.3% over the last year. This reflects trends we’ve seen in recent years when it comes to prices for medicines.
While lawmakers talk about the impact of inflation on American families, the facts show the price of medicines is not part of the problem. But that doesn’t mean patients aren’t hurting at the pharmacy.
According to a recent survey, more than 30% of Americans who have insurance still face a financial barrier to care, including trouble paying medical bills or other out-of-pocket costs. That is due to an insurance system that shifts more and more costs onto vulnerable patients.
- Deductibles and coinsurance account for half of commercially insured patients’ out-of-pocket spending for brand medicines.
- Compared to patients with fixed copays, commercially insured patients with deductibles and coinsurance taking brand diabetes medicines paid 3.6x more out of pocket, on average, in 2019.
- In 2020, brand drug companies provided $187 billion in total discounts, rebates and other payments. But insurers and middlemen known as pharmacy benefit managers (PBMs) often don’t share savings with patients at the pharmacy.
Policymakers spend a lot of time talking about lowering costs by letting the government set the price of medicines. This misguided idea will threaten access to innovative medicines and won’t address the tactics insurers and middlemen use that force patients to pay more for medicines than they should. Instead, we need to work together to make medicines more affordable by capping out-of-pocket costs and making sure the billions of dollars in rebates and discounts get passed on to patients at the pharmacy.
Learn more at PhRMA.org/cost.




